Prior authorization is a crucial process in healthcare that involves the approval of medical treatments or procedures before they are carried out. This process is necessary to ensure that patients receive the right care and that healthcare providers are following the correct procedures. However, prior authorization can be a time-consuming and complex process that requires a lot of paperwork and communication between healthcare providers, insurance companies, and patients.
The prior authorization process for electronic health record (EHRs) consists of five steps:
Determine whether prior authorization is required.
Gather information necessary to support the prior authorization request.
Submit the request for prior authorization.
Monitor the prior authorization request for resolution.
If needed, supplement the prior authorization request with additional required information (and resume at Step 4).
The Da Vinci Burden Reduction project has rearranged these steps for prior authorization into three interrelated implementation guides that are focused on reducing the clinician and payer burden:
Coverage Requirements Discovery (CRD) – This provides decision support to providers at the time they’re ordering diagnostics, specifying treatments, making referrals, scheduling appointments, and so on.
Documentation Templates and Rules (DTR) – This allows providers to download smart questionnaires and rules, such as Clinical Quality Language (CQL), and provides a SMART on FHIR app or EHR app that runs the questionnaires and rules to gather information relevant to a performed or planned service. Running the questionnaires and rules may also be performed by an application that is part of the provider’s EHR.
Prior Authorization Support (PAS) – This allows provider systems to send (and payer systems to receive) prior authorization requests using FHIR, while still meeting regulatory mandates to have X12 278 used, where required, to transport the prior authorization, potentially simplifying processing for either exchange partner (or both).
In this post, we focus on the CRD implementation guide to determine prior authorization requirements and explain how CDS (Clinical Decision Support) Hooks uses AWS HealthLake to determine if prior authorization is required or not.
Solution overview
CRD is a protocol within the electronic prior authorization workflow that facilitates calls between EHRs and the payers using CDS services. When utilized, it provides information on coverage requirements to providers while patient care decisions are in progress. This enables provider staff to make more informed decisions and meet the requirements of their patient’s insurance coverage. Interaction between providers and payers is done seamlessly using CDS Hooks.
CDS Hooks is a Health Level Seven International (HL7) specification. CDS Hooks provides a way to embed additional, near-real-time functionality within a clinician’s workflow of an EHR. With CDS Hooks, eligibility practices like prior authorization can be properly optimized, along with other pre-certification requirements like the physician’s network participation. This function assists providers in making informed decisions by providing them with information on their patient’s condition, treatment options, and the forms that must be completed to facilitate their care. The strategic use of CDS Hooks allows clinicians to quickly develop more patient-centered care plans and assist the prior authorization process by disclosing critical administrative and clinical requirements. For more information on CDS Hooks and its specification, refer to the CDS Hooks website.
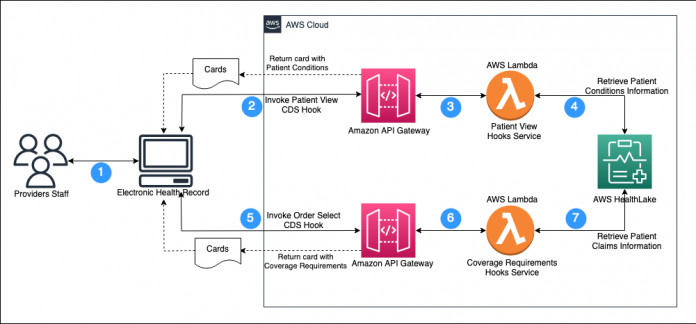
The following diagram illustrates how the CRD workflow is automated using HealthLake.
The workflow steps are as follows:
A provider staff member logs into the EHR system to open the patient chart.
The EHR system validates user credentials and invokes the patient-view hook to retrieve patient condition information.
Amazon API Gateway invokes the Patient View Hooks AWS Lambda function.
The Lambda function validates and retrieves the patient ID from the request and gets the patient condition information from HealthLake.
After reviewing the patient condition, the user invokes the order-select hook to retrieve coverage requirements information for the respective drug.
API Gateway invokes the Coverage Requirements Hooks Lambda function.
The Lambda function retrieves claims information for the patient, runs CQL rules based on the medication submitted and claims information retrieved from HealthLake, and determines whether prior authorization is required.
The solution is available in the Determine Coverage Requirements Discovery using CDS Hooks with AWS HealthLake GitHub repo.
Prerequisites
This post assumes familiarity with the following services:
API Gateway
HealthLake
Lambda
AWS Serverless Application Model (AWS SAM)
Deploy the application using the AWS SAM CLI
You can deploy the template using the AWS Management Console or the AWS SAM CLI. To use the CLI, complete the following steps:
Install the AWS SAM CLI.
Download the sample code from the AWS samples repository to your local system:
git clone https://github.com/aws-samples/aws-crd-hooks-with-awshealthlake-api
cd aws-crd-hooks-with-awshealthlake-api/
Build the application using AWS SAM:
sam build
Deploy the application using the guided process:
sam deploy –guided
# Replace MY_VALUE with proper resource names
Configuring SAM deploy
======================
Looking for config file [samconfig.toml] : Not found
Setting default arguments for ‘sam deploy’
=========================================
Stack Name [sam-app]: aws-cds-hooks-with-healthlake
AWS Region [us-east-1]: us-east-2
#Shows you resources changes to be deployed and require a ‘Y’ to initiate deploy
Confirm changes before deploy [y/N]:
#SAM needs permission to be able to create roles to connect to the resources in your template
Allow SAM CLI IAM role creation [Y/n]:
#Preserves the state of previously provisioned resources when an operation fails
Disable rollback [y/N]:
cdsDemoServicesFunction has no authentication. Is this okay? [y/N]: y
cqlQueryFunction has no authentication. Is this okay? [y/N]: y
cqlQueryOrderFunction has no authentication. Is this okay? [y/N]: y
Save arguments to configuration file [Y/n]: y
SAM configuration file [samconfig.toml]:
SAM configuration environment [default]:
The deployment may take 30 minutes or more while AWS creates a HealthLake data store and related resources in your AWS account. AWS SAM may time out and return you to your command line. This timeout stops AWS SAM from showing you the progress in the cloud, but doesn’t stop the deployment happening in the cloud. If you see a timeout, go to the AWS CloudFormation console and verify the CloudFormation stack deployment status. Integrate CDS Hooks with your clinical workflow when the CloudFormation stack deployment is complete.
Determine coverage requirements for prior authorization
The solution has two hooks, patient-view and order-select, to determine if prior authorization is required or not based on prior authorization rules from payer. CQL is used to evaluate prior authorization rules.
CDS Hooks can be integrated with EHR that supports CDS Hooks. Alternatively, if you don’t have EHR available for testing, you can use the publicly available sandbox as described in the GitHub repo. Note that the CDS Hooks sandbox is being used solely for the purpose of testing.
After your hooks are integrated with EHR, when a user navigates to the clinical workflow, the patient-view hook is run for the configured patient. Note that the patient ID from the clinical workflow should exist in HealthLake. The cards returned from the API indicate that the patient has a sinus infection health condition and the doctor may need to order a prescription.
You can navigate to the RX View tab to order a prescription. Acting as the doctor, choose the appropriate medication and enter other details as shown in the following screenshot.
The order-select hook is returned with the prior authorization eligibility card.
The next step is to submit a prior authorization using the SMART app or other mechanisms available to the provider.
Clean up
If you no longer need the AWS resources that you created by running this example, you can remove them by deleting the CloudFormation stack that you deployed:
sam delete –stack-name <<your-stack-name>>
Conclusion
In this post, we showed how HealthLake with CDS Hooks can help reduce the burden on providers and improve the member experience by determining coverage requirements for prior authorization as part of the prescription order clinical workflow. CDS Hooks along with HealthLake can help providers at the time they’re ordering diagnostics, specifying treatments, making referrals, and scheduling appointments.
If you are interested in implementing a coverage requirement discovery on AWS using this solution or want to learn more about the implementing prior authorization on AWS , you can contact an AWS Representative.
About the Authors
Manish Patel, a Global Partner Solutions Architect supporting Healthcare and Life Sciences at AWS. He has more than 20 years of experience building solutions for Medicare, Medicaid, Payers, Providers and Life Sciences customers. He drives go-to-market strategies along with partners to accelerate solution developments in areas such as Electronics Health Records, Medical Imaging, multi-model data solutions and Generative AI. He is passionate about using technology to transform the healthcare industry to drive better patient care outcomes.
Shravan Vurputoor is a Senior Solutions Architect at AWS. As a trusted customer advocate, he helps organizations understand best practices around advanced cloud-based architectures, and provides advice on strategies to help drive successful business outcomes across a broad set of enterprise customers through his passion for educating, training, designing, and building cloud solutions.
Read MoreAWS Machine Learning Blog